About the Cochlear Implant Center
The Cochlear Implant Center at Westchester Medical Center, flagship of the Westchester Medical Center Health Network (WMCHealth), provides coordinated audiology and speech-therapy services for children and adult cochlear-implant patients and those considering this life-changing technology.
The Cochlear Implant Center is staffed by a team of highly trained audiologists and speech pathologists with expertise in evaluation and rehabilitation services for individuals who are cochlear-implant candidates and those who receive a cochlear implant. Cochlear implantation is a highly successful technology that allows deaf children to hear and speak, and enables deafened adults to enhance their lives. The Cochlear Implant Center provides comprehensive services such as individualized programming of the implant and speech-therapy services.
The Cochlear Implant Center, which has offered cochlear-implant services for 10 years, now is located in a dedicated space at 19 Bradhurst Avenue in Hawthorne, conveniently close to Westchester Medical Center in Valhalla.
The Cochlear Implant Center maximizes leading therapies, technology, equipment and medical research to provide advanced evaluation and treatment. The entire medical team guide patients through care with dignity, compassion and educational information at every step. Each team member embraces the need for nuanced attention from initial consultation through treatment and every step of aftercare. This personal touch is essential: Cochlear Implant Center team members care for each patient the way they would care for their own families.
Chief of Neurotology Katrina Stidham, MD, is Director of Cochlear Implant Center and the Balance Center. She has more than 20 years of experience with cochlear implants. The center’s team offers patient-support groups, educational events and ongoing clinical research to improve our patients' cochlear implant journeys and overall outcomes.
Thank you for trusting the Cochlear Implant Center team and allowing us to be part of your care – and future.
Appointments, Referrals, Information
Physicians: Download Our Patient Referral Form
Cochlear Implant Center
19 Bradhurst Avenue
Suite 3800 South
Hawthorne, NY 10532
914.493.4634
CochlearImplantCenter@wmchealth.org
Directions via Google Maps
American Cochlear Implant Alliance
The Cochlear Implant Center at Westchester Medical Center is a member of the American Cochlear Implant Alliance, a not-for-profit membership organization created with the purpose of eliminating barriers to cochlear implantation by sponsoring research, driving heightened awareness and advocating for improved access to cochlear implants for patients of all ages across the US. Learn more.


What Is A Cochlear Implant?
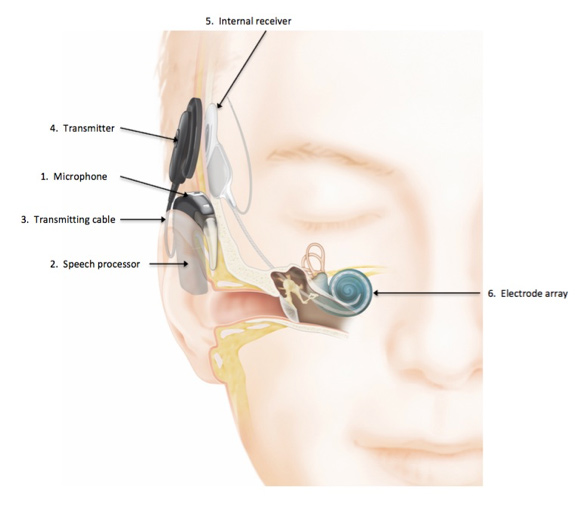
A cochlear implant hearing aid is a specialized device that allows individuals with significant hearing loss to perceive sound and to better understand speech. The cochlear implant electrically stimulates nerve cells in the inner ear (cochlea) which then sends the signals up the hearing nerve to the brain. In doing so, the cochlear implant bypasses the problem affecting people with significant hearing loss that prevents them from benefiting from hearing aids.
How Does A Cochlear Implant Work?
There are two parts to a cochlear implant hearing aid: an external component that consists of a microphone, speech processor and transmitter, and an internal component that consists of a receiver/stimulator and electrode array.
The implant works in the following way:
- The microphone picks up sound and sends it to the speech processor.
- The speech processor analyzes and codes the signal.
- The coded signal is sent to the transmitter.
- The transmitter sends the signal across the skin via a magnet to the internal receiver/stimulator.
- The internal receiver/stimulator sends the signal to the electrode array in the cochlea, which is the spiral cavity of the inner ear. It contains the organ of Corti, which produces nerve impulses in response to sound vibrations.
- The electrode array stimulates the auditory nerve and the signal is sent to the brain.
The internal component is placed by a surgical procedure and is in position at all times under the skin. After surgery, the external component is programmed for the patient. It is worn similarly to a hearing aid; the wearer places the external device in the morning and removes it at night before sleep. The external device is often worn as an ear level processor behind the ear. For very young children, a body-worn processor may be used. Newer speech processors sit entirely on the head, alleviating the need for anything on or in the ear.
Types of Cochlear Implants for Hearing Loss
Some cochlear implants provide only electrical stimulation. Other devices, known as “hybrid” devices, are intended for individuals who have better hearing in the low- and mid-frequency ranges and poorer hearing in the higher frequencies. These devices make use of the user’s natural hearing by providing a low-frequency acoustic signal while stimulating the high frequencies with an electrical signal. The result is a more natural sound and improved speech understanding.
Three Basic Types of Speech Processors
- Over the ear: The speech processor is worn over the ear and connected to a wire and coil that transmit the signal to the internal portion of the device.
- Off-ear-worn device: The speech processor is worn on the body and attached to a long cord that connects to a device on the head. The signal is delivered to the internal piece through the wire and the piece on the head.
- Head-worn device: The speech processor and transmitter are encased in one small device that is placed on the head.

Appointments, Referrals, Information
Cochlear Implant Center
19 Bradhurst Avenue
Suite 3800 South
Hawthorne, NY 10532
914.493.4634
CochlearImplantCenter@wmchealth.org
Directions via Google Maps
Expanded Medicare Coverage for Cochlear Implants
Effective September 26, 2022, the Centers for Medicare & Medicaid Services (CMS) expanded Medicare coverage for treatment of bilateral pre- or post-linguistic, sensorineural, moderate-to-profound hearing loss in qualifying Medicare recipients with hearing test scores between 41-60 percent.
Qualifying criteria includes:
- Diagnosis of bilateral moderate-to-profound sensorineural hearing impairment with limited benefit from appropriate hearing (or vibrotactile) aids;
- Cognitive ability to use auditory clues and a willingness to undergo an extended program of rehabilitation;
- Freedom from middle ear infection, an accessible cochlear lumen that is structurally suited to implantation, and freedom from lesions in the auditory nerve and acoustic areas of the central nervous system;
- No contraindications to surgery; and
- The device must be used in accordance with Food and Drug Administration (FDA)-approved labeling.
Information provided by CMS. Full memo available here.

The Cochlear Implant Center’s specialized services are uniquely customized for each individual to ensure the best outcome. Patients eligible for a cochlear implant include:
- Children 9 months (younger in some cases) to 18 years of age and adults who have moderate to profound hearing loss in both ears and poor speech-understanding skills.
- Adults with mild to moderate low-frequency hearing loss and severe to profound sensorineural-hearing loss who may be candidates for “hybrid” devices.
- Children and adults with profound hearing loss in one ear and better hearing in the other ear may be candidates under the FDA’s new criteria for cochlear implantation in single sided deafness.
- Individuals who receive limited benefit from properly fitted hearing aids.
-
Potential cochlear implant recipients, who have appropriate expectations and are willing to commit to follow-up and therapy as needed.
- Children who have access to appropriate educational and therapeutic resources and a family commitment to adhere to recommendations and follow-up.
- Individuals with no medical restrictions regarding surgery.
Evaluation for cochlear implantation is performed by the cochlear-implant team, which includes these team members:
Neurotologist (Ear Surgeon Subspecialist)
- The neurotologist performs a thorough case history and physical examination.
- The doctor orders radiologic studies, such as a CT scan and/or MRI scan, to evaluate the integrity of the inner ear and auditory nerve.
- The physician may refer you to other medical specialists or for additional testing, as indicated.
-
If approved for cochlear implantation, the neurotologist performs the implant surgery and provides regular medical care for the implant long-term.
Audiologist
- The audiologist performs a basic audiologic assessment to confirm hearing levels.
- Electroacoustic evaluation of your hearing aids determines if they are in good working order and appropriate for your hearing loss. In some cases, you may be fitted with different hearing aids, at least for the cochlear implant evaluation.
- Testing is performed to measure hearing levels with the hearing aids and the ability to understand speech.
Speech/Language Pathologist
- The speech/language pathologist evaluates all children undergoing evaluation for cochlear implantation. The evaluation measures your child’s ability to understand and use spoken language and/or visual methods of communication.
- An evaluation may be recommended for some adults, especially those with a long-standing history of significant hearing loss or those with other neurodevelopmental disabilities.
Team Meeting
- After evaluations are complete, team members meet to discuss the test results and a final determination of candidacy is reached.
- If approved, you will be scheduled to meet with the audiologist to discuss device options.
- You will be contacted by Cochlear Implant Center office staff to discuss possible surgical dates and pre-authorization for surgery.
Appointments, Referrals, Information
Cochlear Implant Center
19 Bradhurst Avenue
Suite 3800 South
Hawthorne, NY 10532
914.493.4634
CochlearImplantCenter@wmchealth.org
Directions via Google Maps

Surgery takes less than two hours for placement of the cochlear implant and testing of the device. Almost all patients go home the day of surgery. You will be given pain medication for expected mild to moderate pain the first few days after surgery.
What Happens After Surgery?
- Most patients return to the physician’s office for a check-up one week later.
- You will not hear until the external portion of the device is activated and “mapped” or programmed. This is usually done three to four weeks after surgery. The mapping sets the device to maximize your ability to hear soft sound and tolerate the new auditory input. The initial appointment is typically two hours long. You will return for a follow-up visit one week later.
- Further mapping is completed monthly to bi-monthly during the first six months and every six to 12 months thereafter.
- Many adult recipients find that they acclimate easier and quicker by participating in aural rehabilitation. The speech-language pathologist will provide activities to help you learn to better use your cochlear implant.
- All children with cochlear implants must receive speech and language therapy and educational support. The cochlear implant team will help select appropriate placements and resources. Our speech/language therapist is available for ongoing therapy and assessment.
Do I Need Additional Listening Equipment?
Many individuals can further improve their ability to understand spoken language by using other types of technology in conjunction with cochlear implants. Some examples may include:
- Amplified and/or closed-captioned phones.
- Remote microphones.
- The three cochlear implant manufacturers have devices that “stream” sound directly from another person or directly from an audio source (such as a TV or radio) to the cochlear implant. These devices improve the user’s ability to hear from a distance and/or to hear in noisy or environments where there is reverberation.
- Bluetooth streaming. Audio output from a Bluetooth-enabled device, such as a cellphone or computer, can be directly streamed to your cochlear-implant speech processor. This allows hands-free talking on the phone and better speech understanding.
- Waterproof options. Waterproof sleeves or covers allow you to use your cochlear-implant speech processor in the bath/shower or when swimming.
Appointments, Referrals, Information
Cochlear Implant Center
19 Bradhurst Avenue
Suite 3800 South
Hawthorne, NY 10532
914.493.4634
CochlearImplantCenter@wmchealth.org
Directions via Google Maps
Success Stories
Music to Her Ears

Fall 2023 Conference

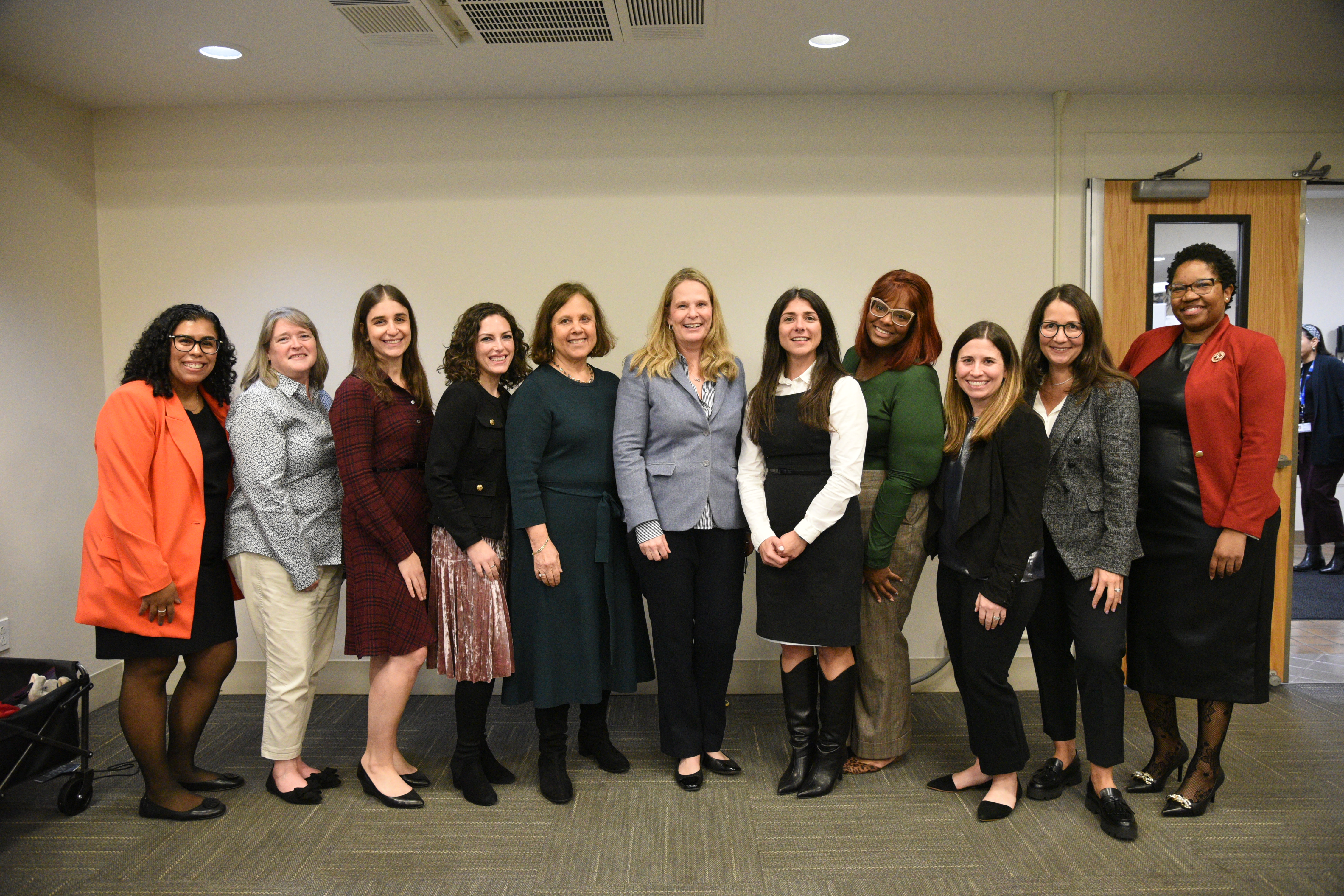



.jpg)


Succeeding At School with Hearing Loss and Cochlear Implants (March 2023)






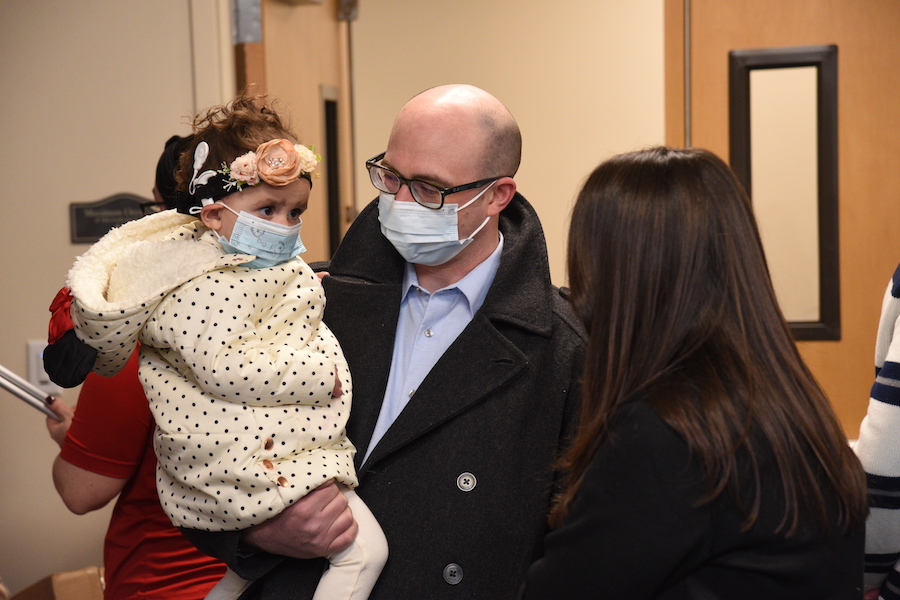


Appointments, Referrals, Information
Cochlear Implant Center
19 Bradhurst Avenue
Suite 3800 South
Hawthorne, NY 10532
914.493.4634
CochlearImplantCenter@wmchealth.org
Directions via Google Maps
The Westchester Medical Center Cochlear Implant Center Team
 |
|
Katrina R. Stidham, MD
Chief of Neurotology
Director, Balance Center and Cochlear Implant Program
Westchester Medical Center
Dr. Stidham is a fellowship-trained neurotologist and skull base surgeon practicing the full scope of otology and neurotology. She also is an Associate Professor of Otolaryngology and Neurosurgery at New York Medical College, the academic affiliate of Westchester Medical Center. Dr. Stidham received her medical degree from the Duke University School of Medicine and completed her surgical residency in otolaryngology - head and neck surgery at Stanford. She completed her neurotology/skull base fellowship at the California Ear Institute at Stanford. Prior to joining the Westchester Medical Center team, she practiced in California for eight years as the medical director of the Cochlear Implant Program at Children’s Hospital Oakland.
Dr. Stidham's scope of practice includes care for children and adult patients with ear and skull base disorders. She has expertise in diagnosis and management of hearing loss, acute and chronic ear disease, dizziness, balance problems, lateral skull base tumors and facial nerve disorders. She has special interests in cochlear implants, congenital hearing loss, pediatric otology, cholesteatomas, vestibular schwannomas, Meniere's disease (inner ear disease), dizziness and otosclerosis.
Dr. Stidham is an American Cochlear Implant Alliance State Champion. She is actively involved in helping to support and promote initiatives of the ACIA to advance access to care for potential cochlear implant recipients.
|
 |
|
Mindy Schmelzer, AuD, CCC-A
Mindy Schmelzer is the Audiology Director at the Westchester Medical Center Cochlear Implant Center and a lecturer in the Graduate Speech/Language Pathology Program at New York Medical College. Her areas of interest include electrophysiologic assessment of hearing, early identification of hearing loss, pediatric hearing aids and cochlear implants.
She received her doctoral degree in audiology from the Salus University School of Audiology and her master’s degree from Arizona State University. She completed her internship at the Veterans’ Administration Hospital in Phoenix and her clinical fellow year at Albert Einstein College of Medicine Hospital.
|
 |
|
Kristi D’Auria, AuD, CCC-A
In addition to her role at the Westchester Medical Center Cochlear Implant Center, Kristi D’Auria is a lecturer in the Graduate Speech/Language Pathology Program and a Clinical Supervisor to fellows and graduate students at New York Medical College, Westchester Medical Center’s academic affiliate. Her areas of interest include electrophysiologic assessment of hearing, early identification of hearing loss, pediatric hearing aids and cochlear implants. She has extensive experience working with children and adults with developmental delays.
She received her doctoral degree in audiology from the Salus University School of Audiology, and her master’s degree from Hunter College. She completed her internship at Columbia Presbyterian Medical Center and her clinical fellowship year at the Head & Neck Surgical Group in New York.
|
 |
|
Rivka Bornstein, AuD, CCC-A, F-AAA
Rivka Bornstein is a clinical audiologist at the Westchester Medical Center Cochlear Implant Center. She conducts a full spectrum of audiologic services including audiologic assessments, electrophyisologic evaluations, and hearing aid and cochlear-implant evaluations. Her areas of interest include electrophysiologic assessment of hearing loss, pediatric assessment of hearing loss, and pediatric hearing aids and cochlear implants.
She received her doctoral degree in audiology from The Graduate Center of the City University of New York in 2010 and her bachelor’s degree in Speech and Communication from Touro College. She completed her fourth-year residency at the Westchester Institute of Human Development.
|
 |
|
Jessica Hoffman, AuD, CCC-A
Jessica Hoffman is a clinical audiologist specializing in pediatric cochlear Implants and hearing aids at the Westchester Medical Center Cochlear Implant Center. She works with all populations performing diagnostic testing, including electrophysiologic assessment of the auditory system. Previously, she worked extensively with two cochlear-implant centers in London, England. In addition, she is a bilateral cochlear implant user and is fluent in American Sign Language.
She received her doctoral degree in audiology from Northwestern University and her bachelor’s degree in Biopsychology from Tufts University. She completed her fourth-year residency at the Westchester Institute for Human Development.
|
 |
|
Samantha Morgan, AuD, CCC-A, F-AAA
Samantha Morgan is a full-time clinical audiologist at the Westchester Medical Center Cochlear Implant Center. She performs electrophysiological and behavioral assessments, as well as cochlear implant and hearing aid services for patients of all ages. She also evaluates auditory processing abilities in children. Her clinical interests include pediatric hearing loss and cochlear implantation, as well as the relationship between hearing loss and cognition in older adults.
She received her doctorate in audiology from the City University of New York Graduate Center and her undergraduate degree in communication disorders from the State University of New York at New Paltz. As a doctoral candidate, she presented original research evaluating the audiological needs of patients with Parkinson’s Disease and taught fellow professionals about the importance of healthcare literacy on a national level. She completed her fourth-year audiological residency at The New York Eye and Ear Infirmary of Mount Sinai.
Samantha is an American Cochlear Implant Alliance State Champion. She is actively involved in helping to support and promote initiatives of the ACIA to advance access to care for potential cochlear implant recipients.
|
 |
|
Michelle Albera, M.S., CCC-SLP, LSLS Cert. AVT
Michelle Albera is a speech language pathologist and listening and spoken language specialist with certification as an auditory-verbal therapist at Westchester Medical Center Cochlear Implant Center. She focuses on listening and spoken language outcomes for children with hearing loss and adult aural rehabilitation. She is a clinical educator for graduate students at WMC and WIHD. Other areas of interest include language learning disabilities, emotional and attentional disabilities as well as reading and writing difficulties. Michelle is trained in the Orton-Gillingham approach to reading.
Michelle received her M.S. in Communication Sciences and Disorders from Emerson College and her B.A. in Speech and Hearing Science from George Washington University.
|
 |
|
Monique McCoogan, Practice Supervisor, Balance and Cochlear Implant Center |
| |
|
Thalian Rojas, Department Coordinator, Cochlear Implant Center |
Appointments, Referrals, Information
Cochlear Implant Center
19 Bradhurst Avenue
Suite 3800 South
Hawthorne, NY 10532
914.493.4634
CochlearImplantCenter@wmchealth.org
Directions via Google Maps